Mandibular advancement devices can help with sleep apnoea in a lot of cases. They are now also provided by the NHS. Find out how exactly they can help, and when they are provided by the NHS.
1. What is a mandibular advancement device?
A mandibular advancement device consists of connected medical-grade plastic arches that are worn on the teeth while sleeping. These push the lower jaw forwards, and with it the tongue and the base of the tongue. Mandibular advancement devices are therefore also referred to as lower jaw advancement devices. They keep the throat and airways clear. This counteracts a very common cause of snoring and sleep apnoea, namely limp base of the tongue slipping backwards into the throat area when sleeping, causing this area to be constricted or even closed.


The mandibular advancement devices can be made of either one or two components.
High-quality devices tend to be made of two components, whereas the entry-level models are usually monobloc devices.


This is not surprising. A comparison of the two device types shows that single-component devices have two key disadvantages compared to two-component devices:
- Firstly, the protrusion cannot be precisely adjusted. The protrusion is set by the user pushing his or her lower jaw forwards when adjusting the device. To change the protrusion setting, the entire adjustment process needs to be repeated. This can quickly lead to material fatigue.
- Secondly, these devices often prevent any lateral movement of the jaw joints. This can quickly lead to jaw joint pain and tension.
| Single-component device | Two-component device | |
| Adjusting the protrusion setting | ||
| Adjusting the protrusion setting |
–
DURING the adjustment process, only possible by re-adjusting the device
|
+
AFTER the adjustment process, variable adjustment without having to re-adjust the device
|
| Adjustment precision | ||
| Adjustment precision |
–
Imprecise (user pushes his or her lower jaw forwards during the adjustment process)
|
+
Precise to very precise, depending on the system
|
| Lateral jaw joint movement | ||
| Lateral jaw joint movement |
–
None
|
–
Low to high (depending on the system)
|
| Mouth breathing | ||
| Mouth breathing |
+/-
Often blocked
|
+/-
Restricted to unrestricted
|
Monobloc devices are, however, suitable if the snoring is caused by two factors at once, namely a constricted throat area plus vibrating soft palate tissue. This is because not only do they keep the throat area clear, but they also prevent mouth breathing that causes the soft palate tissue to vibrate. One key indicator of this type of snoring is the fact that snoring occurs in any sleeping position.
These mandibular advancement devices (two-component) are our customers’ favourites


2. How do mandibular advancement devices work?
Mandibular advancement devices are mainly used by people who snore when sleeping on their back, as well as for position-dependent obstructive sleep apnoea. The term “position-dependent” refers to snoring or obstructive sleep apnoea that occurs at least twice as often when the affected person is on their back compared to when they are on their side.
This is caused by the fact that the base of the tongue becomes limp during sleep and then slips backwards to constrict or close the throat area.
Mandibular advancement devices can help with this. They effectively prevent the tongue from being able to drop backwards into the throat during sleep by moving the lower jaw a few millimetres forwards, thereby applying a slight tension to the tongue muscle. This slight tension means that the tongue muscle is no longer able to drop backwards into the throat. The airways remain free, and you will be able to sleep without any dangerous breathing interruptions or annoying snoring noise.
The image below shows how this works:
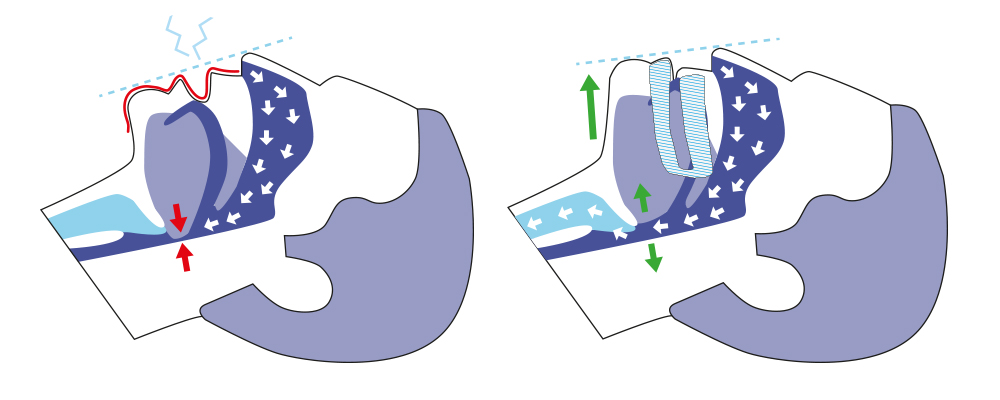
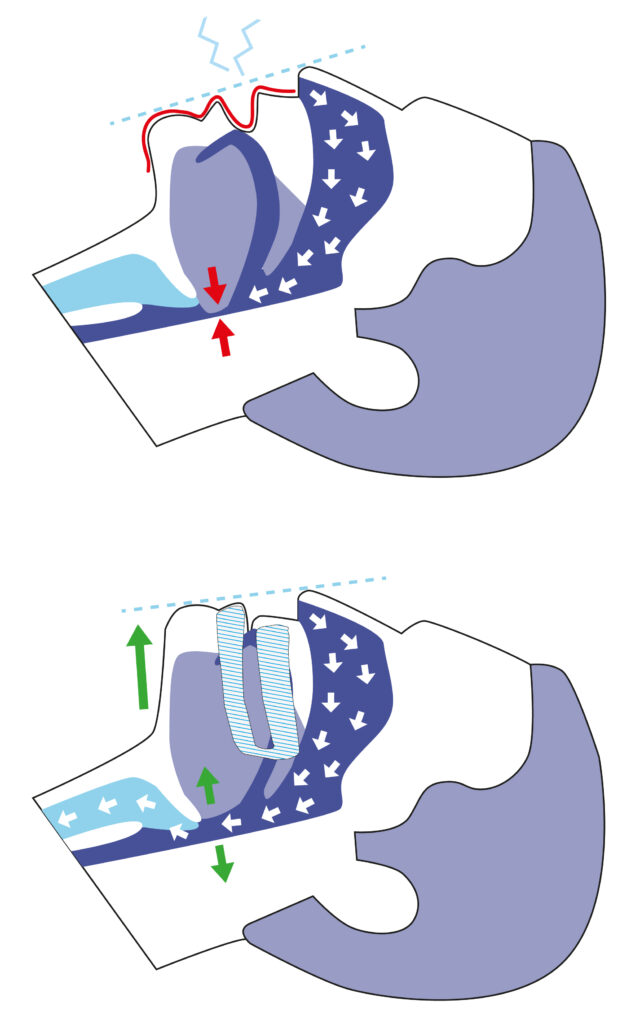
Mandibular advancement devices are a recognised tool against position-dependent snoring and position-dependent sleep apnoea. The effectiveness of mandibular advancement devices against position-dependent obstructive sleep apnoea depends on the severity of the disorder:
- With minor and moderate sleep apnoea, mandibular advancement devices can reduce the number of breathing stops such that the sleep apnoea is no longer categorised as a disease. This is the case when there are fewer than five breathing stops per hour.
- With severe sleep apnoea (more than 30 breathing stops/significant breathing reductions per hour), mandibular advancement devices can significantly reduce the number of breathing stops but are often not able to get this number to below five times per hour. This significantly reduces the severity of the sleep apnoea but the sleep apnoea is not suppressed. In this case, mandibular advancement devices are either used as an additional tool within CPAP therapy in order to reduce the amount of positive pressure that is required, or for patients for whom CPAP therapy is not a suitable option (therapy idea: reducing sleep apnoea is better than not treating it at all).
3. When can a mandibular advancement device be used?
According to our practical experience, there are two conditions that need to be met in order to use a mandibular advancement device:
- There should be ten healthy teeth in both the upper and lower jaws, i.e. a total of at least twenty teeth.
- These teeth should be distributed in the mouth as follows: Five healthy teeth in both the left and right side of the upper jaw, as well as an additional five healthy teeth in both the left and right side of the lower jaw.
Mandibular advancement devices can also be worn if the user has:
- securely anchored bridges, partial crowns or full crowns (although not it these are unstable or in a poor condition)
- securely anchored prostheses and implants (following clarification from a dentist if necessary)
The attending dentist should always be consulted before using a mandibular advancement device if the user
- has loose teeth or unhealthy upper and lower front teeth,
- suffers from jaw pain, serious gum or jaw joint disease or other jaw complaints
- has chronic asthma or epilepsy
- wears braces. bite splints or aligners
4. What are the side effects of mandibular advancement devices?
As with most medical devices, side effects can also occur as a result of using mandibular advancement devices. These may take the form of tooth sensitivity, pronounced salivation or a change in the position of the teeth. Most side effects, however, are only temporary or are easy to fix.
| Side effect of mandibular advancement devices | How can they be fixed? |
| Tooth sensitivity in the mornings | Press the jaw together 3 to 4 times after getting up; tooth sensitivity will usually disappear after this. |
| Feeling of tension in the jaw | Move the teeth back to their “normal state” by:
|
| Pain at the base of the ears | This is a common side effect when first starting to use the device, but usually disappears again quickly. It can also help to reduce the protrusion to start with and then increase it gradually. Exercises that move the teeth back to their “normal state” can also help with this issue (see “Feeling of tension in the jaw”). |
| Pronounced salivation | This issue usually subsides after a few days of regular use.Legt sich üblicherweise nach einigen Tagen regelmäßiger Anwendung. |
| Changes to the interlocking of the teeth in the upper jaw and the teeth in the lower jaw. | See “Feeling of tension in the jaw”. |
5. How much does a mandibular advancement device cost?
This depends on the type of device. A fundamental distinction is made between devices that are produced by a dentist or dental technician (known as customised devices), and mass-produced, off-the-shelf devices:
- Customised devices produced by a dentist cost between around £1200 and £1500.
- Off-the-shelf devices that are certified as medical devices cost between £50 and £150.
This considerable cost difference is down to the very different production methods used for these two types of devices:
- With customised devices, the first step involves creating an impression of the teeth in the upper and lower jaw (either in printed form in as a 3D scan). This impression is used to generate a model in the dental laboratory, which is in turn used to produce the mandibular advancement device. This is then adapted to the user’s teeth by the dentist. The protrusion is then set.
- Off-the-shelf devices are mass-produced from plastic, which can normally be made malleable by being placed in a hot water bath. Once heated and soft, the device is placed on the dental arch and adapted to the teeth. These devices are therefore often referred to as “boil & bite” devices. The protrusion is then set either during or after the adjustment process.
6. Are mandibular advancement devices provided by the NHS?
Does the NHS cover the costs of mandibular advancement devices? As a general rule, a mandibular advancement device will only be provided by the NHS if the snoring is actually classed as a disease. If the snoring is not connected with breathing stops (known as simple snoring), it is not classed as a disease. In this case, the NHS will generally not cover the costs of a mandibular advancement device.
If obstructive sleep apnoea has been diagnosed, on the other hand, the NHS will cover the costs of the mandibular advancement device.
There are three key conditions for this NHS provision:
- An initial assessment of need and a prescription by a secondary care NHS consultant are requirements.
- The patient’s oral health must have been assessed by a dentist.
- The provided mandibular advancement device may take the form of a customised, laboratory-produced device (band 3), which is adjusted and monitored by a dentist. Off-the-shelf devices (band 2) are also provided by the NHS. The applicable dental charges must be taken into account.
Snoring mouth guards – our comprehensive guide
Snoring mouth guards are a popular way of preventing snoring and sleep apnoea. You can find out how they work in our guide.
Mandibular advancement device comparison
All our mandibular advancement devices compared based on comfort, application, cleaning and much more.
Dr. Daniel Grätz is the Managing Director of health.On Ventures GmbH, one of Germany’s leading online providers of snoring mouth guards, and has been providing customers with advice about these devices for many years.









