Snoring can be much more than just a relationship killer or an everyday problem. Here you will learn that you should consult a doctor if you suffer from apnea, i.e. lapses in breathing.Obstructive sleep apnea syndrome (OSAS), upper respiratory tract resistance syndrome (UARS) and central sleep apnea (CSA). Do you suffer from a sleep related breathing that causes snoring? We explain what these conditions are and offer advice and solutions.
Defining: Abnormal snoring
Medicine classifies snoring as pathological if the development of noise is the result of, or accompanied by, a sleep related breathing disorder. This means that the body is not sufficiently or optimally supplied with oxygen during sleep. Here is a brief explanation of how these diseases differ from one another and what needs to be taken into account:
If the upper airways close completely during sleep, i.e. if the tissue in the airways collapses and prevents air from flowing through at all, it is referred to as complete obstruction or obstructive sleep apnea (OSA). A lapse in breathing occurs (apnea) – for a period that can last from a few seconds to more than a minute. During this time no air gets through to the lungs (and no air exits the lungs). The lungs actually “pump”, i.e. the affected person shows breathing movements ( their chest lifts and lowers) but they are unable to breathe. OSA is the most common form of sleep related breathing disorder.
Obstructive sleep apnea vs Obstructive sleep apnea syndrome – What is the difference?
Although the two terms are used synonymously – there is a subtle difference. Obstructive sleep apnea (OSA) is the disease, i.e. the obstruction of the upper respiratory tract during sleep that causes the partial pressure of oxygen in the blood to drop. Obstructive sleep apnea syndrome (OSAS), on the other hand, occurs when the main symptoms of snoring, i.e daytime sleepiness and loss of performance also occur in patients with OSA.
Hypopnea
If, on the other hand, only a partial closure of the upper respiratory tract occurs during sleep, a so-called partial obstruction or hypopnea is present. The tissue also collapses, but only partially. Part of the normal air flow sis still delivered to the lungs, resulting in shallow breathing. However, an oxygen deficiency can also occur here, because the affected person has to breathe in against a resistance during sleep.
Hypopnea syndrome vs. UARS (Upper Airways Resistance Syndrome) – what is the relationship between these diseases?
Hypopnea syndrome vs. UARS (Upper Airways Resistance Syndrome) – what is the relationship between these diseases?
Central Sleep Apnea
Central sleep apnea is a sleep-related respiratory disorder that don’t involve the upper respiratory tract. These primarily include central sleep apnea (CSA). For them, breathing comes to a standstill because the respiratory centre in the brain no longer responds to the respiratory muscles. In purely CSA the upper respiratory tract does not play a role. Therefore there are no snoring noises. Unlike obstructive sleep apnea, central sleep apnea does not involve breathing movements. There is a complete cessation in breathing, the lungs cease to function completely, and not even the chest moves! CSA, however, occurs very rarely.
Mixed forms of central and obstructive sleep apnea syndrome
A sleep related breathing disorder can also present itself in a mixed form. In mixed apnea, a longer central phase (complete respiratory arrest because the respiratory centre in the brain stops functioning) is followed by a short obstructive phase of apnea or hypopnea (because the airways also collapse as a result of respiratory arrest).
The complex sleep apnea syndrome (CompSAS) also falls into the category of mixed forms of sleep apnea. CompSAS patients initially show all symptoms of obstructive sleep apnea and are treated accordingly – often with CPAP therapy. This eliminates the obstruction of the upper respiratory tract. However, these patients then experience symptoms of central sleep apnea. According to a US study, CompSAS could be present in up to 15% of all obstructive sleep apnea syndrome patients.
Consequences of Apnea and Hypopnea
All forms of apnea and hypopnea have one thing in common: they can pose a real danger to the affected person – especially if they are not detected and treated at an early stage. According to studies, the known long-term risks for obstructive sleep apnea syndrome include high blood pressure, stroke and coronary heart disease.
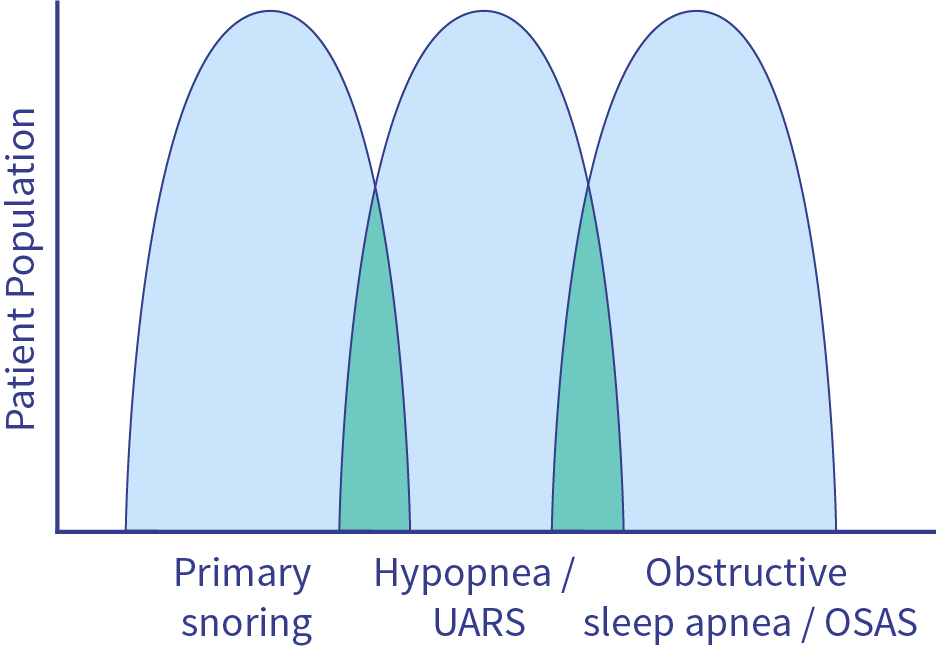
The transitions between different forms of snoring and breathing-related sleep disorders are fluid.
This is why a “snoring career” can also develop dynamically. The simple snorer of today can, over time, become a upper airway resistance syndrome snorer and even end up suffering from obstructive sleep apnea syndrome. This “career development” is not a firmly established path, but it does happen.
What does apnea actually mean?
Apnea comes from the Greek ápnoia and means “non-breathing” (from pnea: ‘breathing’ / ‘breath’) and refers to a more or less prolonged interruption of breathing. In contrast to competitive apnea- or free-diving – where breathing is consciously stopped – sleep apnea causes unconscious, sudden lapses (apnea) in breathing during sleep. The correct pronunciation of apnea involves three syllables: “apˈniːə”.
Sleep Related Breathing Disorder
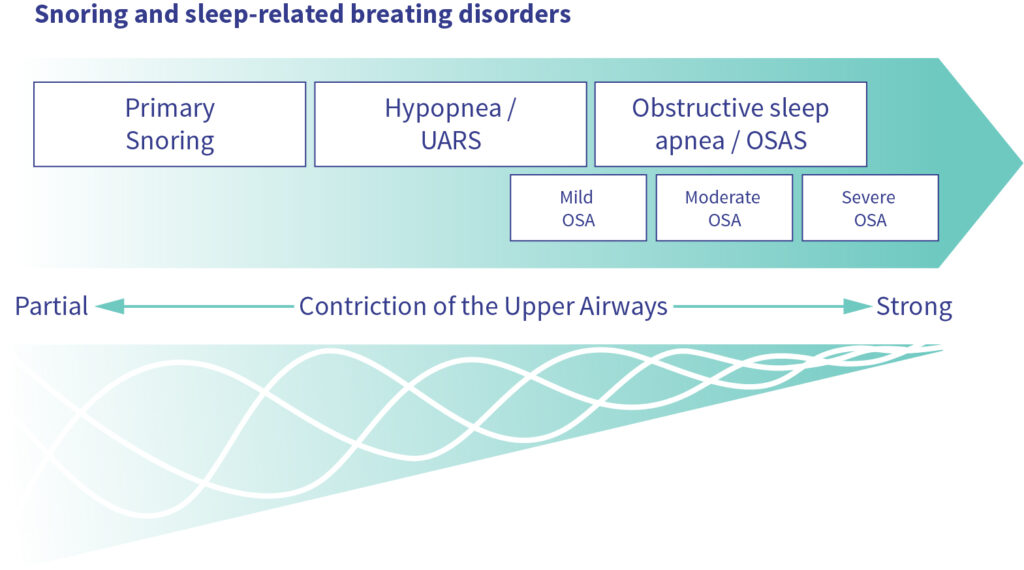
How do I know if my snoring is a health risk?
In order to assess whether you suffer from a sleep related breathing disorder and your snoring is a health risk, you need to find out what type of snorer you. There are different types of snorers and we will explain how you can recognise them. We also tell you how to stop snoring.
Obstructive sleep apnea (OSA Apnea)
OSA apnea occurs when the upper respiratory tract closes partially causing either mild OSA or moderate OSA or closes completely causing severe OSA during sleep at recurring intervals and the oxygen content in the blood drops as a result. We explain the causes and the potential treatment options, especially CPAP therapy.
Did you know that we all experience apnea phases during sleep?
Even in healthy people the respiratory drive is suppressed during sleep. In particular in the REM phase sleep apnea occurs in healthy people. However, as long as the breathing interruptions only occur intermittently and these occurrences are isolated, they do not impair the oxygen supply to the body and are therefore usually benign.
Oxygen saturation
The critical point with OSA apnea is the so-called oxygen desaturation of the blood. Desaturation occurs when too little oxygen enters the lungs via the airways – in other words, when the airways are blocked. The longer the blockage occurs and the more extensive the blockage is, the less oxygen reaches the body and the lower the blood oxygen levels drops. In order to better assess how serious sleep apnea actually is, the medical profession has developed a measurement method and established threshold values.
Apnea-hypopnea index
The so-called apnea-hypopnea index (AHI) indicates how many apnea (complete breathing interruption) and hypopnea (partial breathing interruption) episodes, that last more than 10 seconds per episode, an affected person experiences, that result in an arousal (brief awakening) and / or cause a decrease in blood oxygen saturation levels per hour of sleep. To put it simply: How often does the affected person have to struggle for air in an hour of sleep? The values can then be used to assess the degree of oxygen desaturation of the blood and how severe the obstructive sleep apnea is.
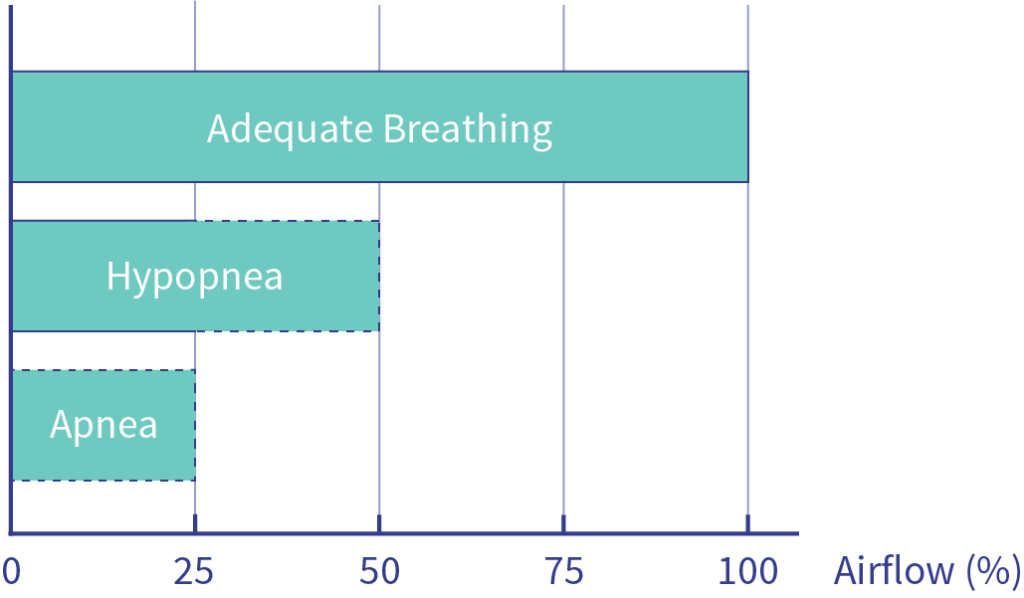
Apnea occurs when airflow is reduced by at least 75% over a period of 10 seconds or more, compared to normal breathing, and results in a blood oxygen saturation level decrease of more than 4%.
Hypopnea occurs when airflow is reduced by 50-75% compared to normal breathing. Blood oxygen saturation levels are not necessarily affected.
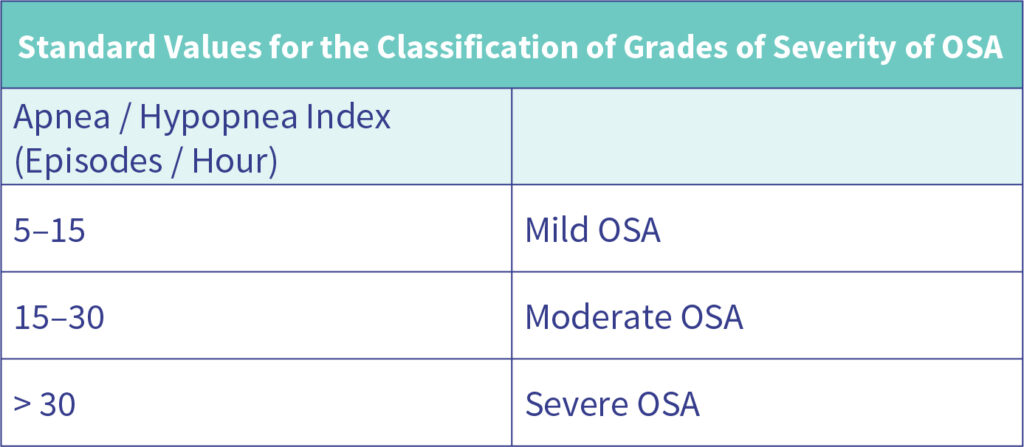
Grading the severity of obstructive sleep apnea
On this basis, the American Society for Sleep Medicine (AASM) has established the following guidelines for determining the severity of obstructive sleep apnea:
What happens during an apneic episode?
Depending on the severity of the OSA apnea ‘’episodes’’ can occur many times per night and follow a recurring pattern. Initially, the muscles and tissue in the upper respiratory tract slacken during sleep. The flabby tissue slides back into the throat and narrows or closes the respiratory tract, thus blocking the airflow. No air (and therefore no oxygen) arrives in the lungs. As a result, the oxygen content in the blood begins to sink – the so-called oxygen desaturation begins. The body registers this reduction and reacts.
How does one start breathing again?
According to a study on arousal , due to a spontaneous wakening reaction, an arousal, – the affected person is startled without waking up completely. As a result, the muscles in the body tense up, this includes the muscles of the upper respiratory tract. The collapsed tissue in the respiratory tract tightens itself, the air can flow again and the oxygen content in the blood normalises. The person sleeps calmly again and the muscles begin to relax. The whole cycle starts all over again!
This sequence of (1) relaxation of the tissue resulting in apnea, (2) oxygen desaturation of the blood, (3) arousal reaction, (4) tightening of the tissue and (5) increase of blood oxygen saturation levels can repeated many times per night.
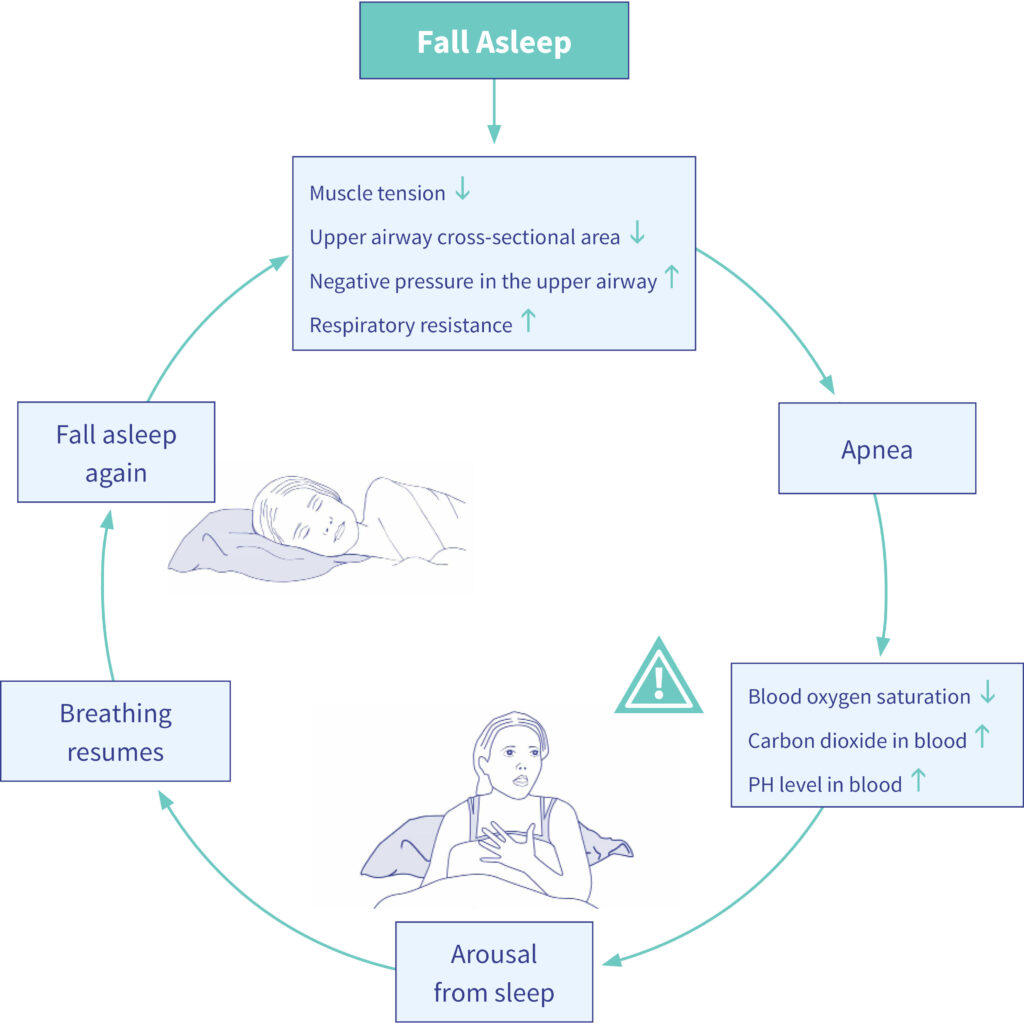
Position-dependent vs. non-position-dependent OSA apnea – What is the difference?
The first way OSA apnea occurs is tongue-based : the back part of the tongue muscle slides backwards into the throat, covers the opening of the oropharynx (throat) and blocks the airway. This form of OSA apnea only occurs while sleeping on the back, when the base of the tongue slides downwards due to gravity gravity. Thus it is called position-dependent OSA apnea. This form of OSA apnea represents approx. 35% of all OSA apnea patients.
Treatment options
Snoring mouthpieces or positional therapy (in the case of mild OSA to moderate OSA), or CPAP masks – if severe OSA is present – provide a remedy for this form of OSA apnea . In addition to these snoring aids, there is also the possibility of solving the problem with an implant, a so-called “tongue pacemaker”.
Other causes of OSA apnea
On the other hand, OSA apnea can occur when the tissue in the pharyngeal region slackens. At this point, the pharynx can be imagined as an elongated tube with muscles in its wall that keep it taut. If these muscles slacken, the tube collapses. Now no more air can flow through the tube. It results in the closure of the respiratory tract. This form of OSA apnea is called most common form.
EPAP vs CPAP Therapy
Mild OSA to moderate OSA forms of non-positional OSA apnea can treated either with EPAP (expiratory positive airway pressure) therapy or with CPAP therapy (continuous positive airway pressure therapy), but severe OSA can only be treated by means of CPAP therapy.
In order to achieve the optimal treatment result, it is important to know – among many other parameters – whether one’s own sleep apnea is position-dependent or not.
Consequences of OSA apnea
Once you have witnessed how dramatically a person suffering from sleep apnea has to struggle for air and oxygen during sleep, you will quickly understand that OSA apnea costs the body a lot of energy and drain it in the long run (here is a short YouTube clip to illustrate this struggle for air). Instead of resting during sleep, the body has to work hard night after night. If this permanent stress remains untreated, it can have dramatic consequences for health.
Not just a lack of sleep
The constant arousal reactions prevent the affected person from reaching the deep sleep stage and thus from getting a restful nights sleep. One experiences daytime fatigue , exhaustion and a lack motivation to perform the following day. People who suffer from OSA apnea are often irritable, permanently feel tired and drowsy, which significantly reduces their quality of life. Personality changes and depression often occur. Their sex life also suffers due to declining libido. Affected men also often have a low testosterone level, which is accompanied by reduced sexual desire and erectile dysfunction.
High blood pressure
Chronic high blood pressure (hypertension) can be a possible long-term consequence of OSA apnea. Normally, blood pressure drops by 10 to 15 percent during sleep. In apneic snoring, however, the systemic blood pressure remains at, or even exceeds, the pressure level whilst awake. In this context, a USA study has found that the chance of suffering from high blood pressure in a person with moderate OSA (AHI of 15 / h or higher) is almost 3 times higher than in a person with healthy breathing. As a result of the high blood pressure, other diseases can develop, because the high pressure strains the entire vascular system of the body. Cracks in and thickening and hardening of the vascular wall are potential consequences. High blood pressure is the main risk factor for arteriosclerosis, which in turn can lead to heart attacks, strokes and other vascular diseases.
Heart Failure
OSA apnea is also suspected of promoting the increased formation of deposits in the coronary arteries. A 2009 Canadian study found a significant correlation between obstructive sleep apnea and the amount of deposits in the coronary arteries. In addition,OSA apnea could also have a negative effect on heart function.
Evaluations of the American Sleep Heart Health Study have shown that men with severe OSA apnea (AHI > 30) have an approximately 60% higher incidence of heart failure than patients with very low OSA apnea values (AHI < 5).
Stroke
In the course of evaluations of the Sleep Heart Health Study mentioned above, a possible link between OSA and stroke risk was also established. According to this OSA apnea-hypopnea study , the risk of stroke in mild OSA to moderate OSA patients (AHI 5-25) should increase by 6% with each additional AHI episode. In further obstructive and central sleep apnea studies
it was shown each (recurring) episode of breathing interruption (apnea) more per hour would increase the risk of a stroke by 6%. OSA apnea is also associated with cardiac arrhythmias. Finally, it is also suspected that OSA apnea promotes certain metabolic diseases, in particular diabetes mellitus. An oxidative stress study
has, however, not yet concretely proven how the increased insulin resistance of OSA apnea patients is caused.

OSA apnea and driving – a highly dangerous combination!
There are numerous studies that have investigated the effects of OSA apnea on road safety. These studies show that OSA apnea patients are 2-3 times more likely to be involved in a car accident than healthy sleepers (other studies even show a 6-fold higher risk). Thus OSA apnea is not only dangerous for the affected persons themselves, but also for all other participants in road traffic. One more reason to take the disease seriously and to handle it responsibly.
How do I know if I have OSA apnea?
Only a doctor can give an unambiguous diagnosis of obstructive sleep apnea. However, there are a number of symptoms of which you, as a patient, need to be vigilant. You should consult a doctor (ENT / sleep specialist) for further clarification, if you
(1) suffer from marked daytime fatigue without any recognisable cause and
(2) snore loudly at night and have to gasp for air again and again (i.e. your breathing is interrupted), if you wake up repeatedly at night, if you have feel unrested after sleep or if your ability to concentrate is reduced.
Self-test: Am I at risk for obstructive sleep apnea?
If you suspect that OSA may be a problem for you, you should do the so-called ESS test (Epworth Sleepiness Scale-Test). You can complete and evaluate the test yourself. All you have to do is answer eight questions about daytime drowsiness and the tendency to fall asleep. You can access the ESS test here .
A total score of less than 6 is inconspicuous, for values between 7-9 it is recommended that you consult an expert (ENT / sleep specialist). If you achieve a result of more than 10 points, you are very likely to suffer from a sleep-related respiratory disorder. You should definitely contact an ENT or sleep specialist.
Apneic snoring
Apneic snoring also has a specific sound pattern that can easily be recognised: There is an alternation between snoring and silence. The snoring itself is often very loud and disturbing and breathing is regularly interrupted (apnea) for several seconds during which the snorer stops breathing. The respiratory interruption often ends with a loud grunt when the body struggles for air and the airways open again.
Sleep amnesia
Whether an affected person can remember these “suffocation attacks”, however, is not a reliable indicator. This is because the affected snorer often only experiences breathing interruptions unconsciously, i.e. in most cases he does not wake up from them, but only briefly jerks awake up during sleep. Just because someone can’t remember suffering from breathing interruption during sleep doesn’t they don’t suffer from apnea.
Symptoms of OSA apnea
In addition, there are a number of other symptoms of OSA apnea that are not meaningful on their own. These include sleep without restorative value, morning headaches, dry mouth, reduced attention thresholds, confusion in the morning, mood swings, depression, high blood pressure, reflux of gastric fluid or sexual dysfunction ranging from a reduction in libido to impotence.

The golden rule: If you have evidence that you may be suffering from OSA apnea (OSAS), contact your family doctor or a specialist (ENT / sleep specialist) as soon as possible. OSA apnea is a serious condition and should be investigated by a doctor.
I suffer from OSA apnea – What can I do?
If you have been diagnosed with OSA apnea by a sleep laboratory or a sleep specialist, this is usually accompanied by a treatment recommendation. CPAP therapy is the standard recommendation in these instances. It still represents the therapeutic gold standard today, as all forms of OSA apnea can be effectively treated with it.
However, many patients perceive this therapy as a severe restriction of their quality of life or sleep. After all, one sleeps with a ventilation mask and is exposed to a continuous, motor-generated air flow. Because of these disadvantages, many patients discontinue therapy completely or do not use it regularly. Many are also looking for an alternative to CPAP therapy. These alternatives actually exist, but not for every form of OSA apnea! Here is an overview:
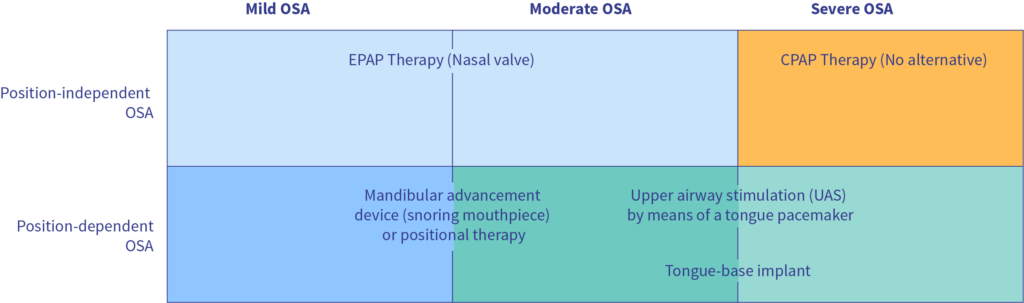
CPAP therapy alternatives
EPAP therapy
EPAP therapy (“nasal valves“) are available as an alternative to CPAP therapy for mild OSA and moderate OSA that are not position-dependent.
Mandibular advancement devices
In position-dependent OSA apnea , both mild OSA and moderate OSA can be treated with mandibular advancement devices (snoring mouthpieces) or positional therapy. Mandibular advancement devices (MADs) are worn at night and push the lower jaw forward. This prevents the tongue from sliding into the back of the throat.
Positional therapy
Positional therapy belts and vests make sleeping in supine position (i.e. on the back) totally uncomfortable and thus promote sleep in the lateral (i.e. on the side) and prone (i.e. on the stomach) position. In these sleeping positions, the tongue remains in its original position.
UAS stimulation therapy
Alternatively, an implant in the base of the tongue (UAS stimulation therapy of the upper respiratory tract) could be considered for position-dependent OSA apnea . By means of short electrical impulses, it prevents the base of the tongue from slackening during sleep and thus from sliding back into the throat and blocking the airway.
Do you suspect you suffer from OSA apnea
If you only suspect that you may be suffering from OSA apnea, you should seek medical advice. A doctor specialising in OSA apnea will advise you how to proceed. Generally you will be advised to participate in a home sleep study. You will be given a small box to take home with you, which records certain sleep and breath related body data and can be read by your doctor after a few days of use.
What happens if your suspicions are confirmed?
If the suspicion of OSA apnea is confirmed, a polysomnographic examination would follow. This means that you will spend one night a sleep laboratory, where a variety of data relating to your sleep and breathing behaviour will be measured. On the basis of this data (and previous medical examinations) the sleep specialist can then determine whether or not you are actually suffering from a breathing-related sleep disorder (the main case of which is: obstructive sleep apnea). You will then receive a diagnosis and therapy recommendation.
Hypopnea – Upper Airway Resistance Syndrome – Central Sleep Apnea
Sleep related breathing disorders are complex and have a disruptive effect on one’s daily life. The difference between the different types of sleep related breathing disorders; hypopnea syndrome, upper airway resistance syndrome and central sleep apnea are confusing, especially if you suffer from mixed apnea. We clarify the difference and offer advice on how to treat these conditions so that you can lead a normal, productive life.
Hypopnea syndrome could be described as the “baby brother” of obstructive sleep apnea. It is a breathing-related sleep disorder during which only hypopnea occurs. In its pure form it occurs quite rarely, in most cases both apnea and hypopnea occur. Together, their interaction obstructive sleep apnea hypopnea syndrome (OSAHS), can have a similarly stressful effect as pure apnea. This circumstance also caters toward the most widespread method of measuring breathing-related sleep disorders, viz. the AHI (apnea-hypopnea index), since it does not differentiate between apnea and hypopnea, but only records the total number of episodes (or “incidents”).
What is hypopnea?
Hypopnea leads to a reduction in airflow, but not to a total respiratory standstill. This is where hypopnea differs from apnea, in which airflow (almost) comes to a complete standstill. The consequence of hypopnea is that the individual has to make an increased effort to breathe, whilst sleeping, since only 25-50% of the normal airflow reaches the lungs. In the long run, pure hypopneas can also put a heavy strain on the body, because they can also lead to a change in the heart rate and to spontaneous waking reactions (arousals) – although these consequences occur less frequently than with apnea.
What is the diagnostic criteria for hypopnea?
This is not uniformly determined. The American Society for Sleep Medicine (AASM), for example, defines two alternative characteristics:
(1)a reduction of airflow by at least 50% of the initial value over a period of at least 10 seconds plus oxygen desaturation of the blood by at least 3% or the presence of a spontaneous arousal reaction or
(2) a reduction of the airflow by at least 30 % of the initial value over a period of at least 10 seconds plus oxygen desaturation of the blood by at least 4 %.
How can I tell if I suffer from hypopnea?
Hypopnea and apnea are often difficult to distinguish. That is why what is said about obstructive sleep apnea syndrome also applies
(1) marked daytime drowsiness with no discernible cause, and
(2) loud night snoring combined with repeated gasping for air or you feel unrested after sleep or experience reduced concentration.
What can I do if I have Hypopnoea Syndrome?
In principle, the same recommendations apply as for obstructive sleep apnea.
Upper Airways Resistance Syndrome (UARS) is also a breathing related sleep disorder disorder. Put simply, it is right in the middle between simple, benign primary snoring and pathological obstructive sleep apnea (OSA). With upper airway resistance syndrome there are recurring so-called “incomplete obstructions” of the upper respiratory tract. This means that although the airways remain open at all times, they can narrow considerably and thus impair or reduce the flow of air. Upper airway resistance syndrome patients have no apnea (respiratory arrest), but a normal oxygen saturation in the blood. In other words, they are supplied with sufficient oxygen at all times. This is where upper airway resistance syndrome differs significantly from obstructive sleep apnea.
Spontaneous arousal reactions – The “littlest common evil”
Obstructive sleep apnea syndrome (OSAS) and upper airway resistance syndrome patients both suffer from spontaneous “arousals” at night. These waking reactions prevent a healthy structured sleep and thus lead to daytime fatigue and general exhaustion. When and how the arousal reactions occur differs in both diseases, however. While the upper airway resistance syndrome patient, who has a comparatively mild respiratory impairment, is shocked by the slightest amount of extra strain required to restore breathing to normal and thus suffers an arousal reaction. The Obstructive sleep apnea syndrome patient only reacts when they are suffering from a significant oxygen deficiency.
What triggers an arousal?
The trigger for the spontaneous arousal reaction in obstructive sleep apnea syndrome is the drop in the the oxygen saturation level of the blood. The brain registers this drop and counteracts it with the arousal reaction. In upper airway resistance syndrome, however, the trigger is an increased workload, the body registers that breathing has become more difficult. The reason for this is that the lungs have to breathe in against increased resistance caused by the narrowing of the upper respiratory tract. With upper airway resistance syndrome, however, the body is sufficiently supplied with oxygen at all times. Due to the frequent arousals, upper airway resistance syndrome patients show a persistently disturbed “sleep architecture”.
How is upper airway resistance syndrome diagnosed?
The diagnostic criteria for upper airway resistance syndrome are not standardised – partly because the disease of its own, partly because it is a variant of obstructive sleep apnea syndrome (“as part of a continuum between primary snoring and obstructive sleep apnea”). As a consequences of upper airway resistance syndrome, the cardiovascular burden of upper airway resistance syndrome is considerable, because the affected person has to breathe in against a high resistance with upper airway resistance syndrome.
Breathing into a vacuum
Despite the bottleneck in the upper respiratory tract, the patient still has to inhale sufficient air and oxygen into the lungs – in other words, the body has to exert itself and increases breathing performance. As a result, the negative pressure (“vacuum”) in the chest increases (so-called negative intrathoracic pressure). This value can be as low as -100 mbar. This would correspond to the value that can occur with a complete airway occlusion in the context of obstructive sleep apnea.
Consequences of upper airway resistance syndrome
According to a upper airway resistance syndrome study it is therefore also suspected that it leads to comparable pathological changes in the heart, circulation and sleep quality as obstructive sleep apnea syndrome. The high negative intrathoracic pressure (pressure in the chest) is also partly responsible for upper airway resistance syndrome patients suffering from increased reflux (reflux of gastric fluid).
Predisposing conditions
Upper airway resistance syndrome is comparatively common in patients of normal weight and young age. In addition, women are more often affected by upper airway resistance syndrome than by obstructive sleep apnea syndrome. Upper airway resistance syndrome also occurs more frequently in the third trimester of pregnancy. Because expectant mothers don’t only gain weight in the abdominal area, but also around the neck and throat area. Fatty deposits in the respiratory tract favour constrictions and impairments of breathing.
Evolution of upper airway resistance syndrome
Upper airway resistance syndrome can change to obstructive sleep apnea syndrome if you gain weight. It is to some extent a precursor to obstructive sleep apnea syndrome and can progress if not detected and treated.
How can I tell if I have UARS?
Unrecognised sleeping disorder
Upper airway resistance syndrome has the reputation of being an “unrecognised sleeping disorder”. The disease is by far not as well known as OSA and cannot be detected with a doctor’s standard diagnostic tools because it does not lead to breathing interruptions (apnoea) or to oxygen desaturation of the blood.
Home sleep studies do not deliver any significant results. UARS can only be tracked by using measuring methods that also register cyclic pressure changes within the chest (such as polysomnography analysis in a sleep laboratory). The typical respiratory event in patients with upper airway resistance syndrome is called RERA (respiratory effort-related arousal).
Differential diagnosis
If you suffer from the following complaints and obstructive sleep apnea has been ruled out, you should at keep upper airway resistance syndrome in mind differential diagnosis: excessive daytime drowsiness, fatigue and sleep fragmentation, people with upper airway resistance syndrome also battle to fall asleep and to sleep-through, they suffer from anxiety and experience gastric reflux.
It is also important to know that upper airway resistance syndrome patients do not always snore. They often attribute their excessive fatigue to stress or other external factors.
What can I do if I suffer from Upper airway resistance syndrome?
As with OSA, ventilation therapy using a CPAP device is the standard therapy for upper airway resistance syndrome. However, CPAP therapy is not well accepted by upper airway resistance syndrome patients because it makes the typically severe sleep problems of upper airway resistance syndrome patients even more difficult. This is why upper airway resistance syndrome very often uses alternative therapies. EPAP therapy (“nasal valves”) can be considered as an alternative for upper airway resistance syndrome in any position. People who suffer from position-dependent upper airway resistance syndrome responds well to treatment with snoring mouthpieces (mandibular advancement devices) or positional therapy.
In children with upper airway resistance syndrome, the removal of enlarged tonsils may be considered.
Central Sleep Apnea (CSA)
Central sleep apnea occupies a special position among the breathing related sleep disorders. It is not caused by narrowing or obstruction of the upper respiratory tract, but by damage to the respiratory centre in the brain. The central nervous system virtually “forgets” to activate the respiratory muscles and as a result respiratory arrest occurs. Respiratory control does not function reliably. People affected by central sleep apnea do not really “snore”, but they do experience breathing interruptions. This “silent” interruption of breathing is therefore often not registered by their bed partner. As a result many central sleep apnoea cases are not recognized and not treated.
Often respiratory arrests are also accompanied by an increased respiratory drive. The body wants to compensate the under supply by following up with increased breathing activity – which results in the patient breathing more intensely, than necessary. This periodic pattern of increasing and decreasing breathing effort and respiratory flow is characteristic for, so-called, Cheyne-Stokes Respiration, the best known form of central sleep apnea.
Central sleep apnea patients experience repeated arousal reactions during sleep and therefore suffer from interrupted sleep and, as a consequence, from daytime drowsiness, concentration difficulties and poor performance. Risk factors for central sleep apnea are cardiac insufficiency, renal insufficiency, circulatory disturbances of the brain or even life in high altitudes.
Central sleep apnea is primarily treated by treating or curing the underlying disease (heart failure, renal insufficiency etc). In many cases, this is done through drug therapy.
In the past attempts were made to correct the breathing pattern in Cheyne-Stokes respiration using ventilation therapy so that it corresponded to natural, constant breathing. However, recent studies (SERVE-HF) have shown that this practice produces the opposite effect. Instead of helping – i.e. increasing life expectancy and quality – the use of ventilation therapy led to a higher mortality rate of patients. The causes for this are not yet clearly understood, but it is possible that patients with heart defects need nocturnal apnea as a protective mechanism.
Central sleep apnea and obstructive sleep apnea can also occur together – as mixed apnea. The cause of respiratory arrest is always the lack of impulse from the central nervous system. This is followed by a physical collapse of the upper respiratory tract.
This unique CPAP mask test compares the most popular masks on the market. einander gegenüber
The most important purchasing criterion for mask wearers; comfort, freedom of movement and far more, coherently summarised especially for you.
How do I find the right CPAP mask?
Discover how you find the right CPAP mask and what you should pay attention to.
The best snoring mouth guards
There are five anti-snoring mouthpieces that our SomniShop customers liked the most. Find out which ones they are!

Medical Doctor, Berlin
Jan Wrede works as a medical doctor in Berlin. He studied medicine at FAU University in Erlangen-Nuremberg and Semmelweis University in Budapest. He had already written numerous scientific articles during his studies, especially on the subject of snoring.







 Welcome to SomniShop
Welcome to SomniShop